- Home
- Health Center
- Health Info
- Adjusting To Life With Type 2 Diabetes Or Prediabetes
Adjusting To Life With Type 2 Diabetes Or Prediabetes

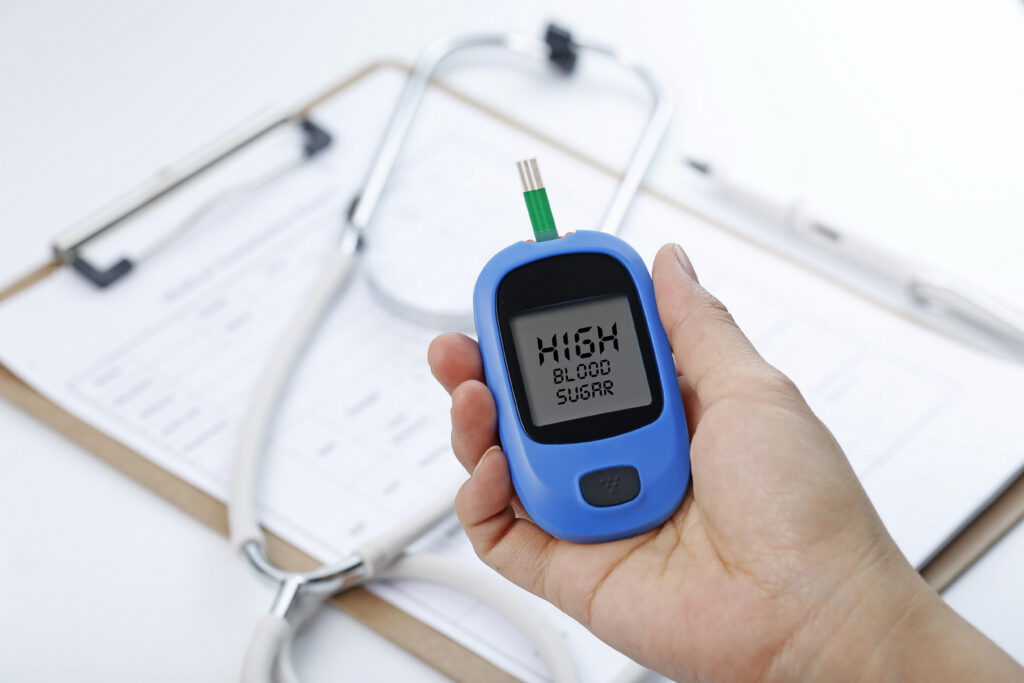
What is type 2 diabetes?
Diabetes means that your blood glucose (also called blood sugar) levels are elevated. This is also called hyperglycemia.
The digestive tract breaks down carbohydrates from the food you eat into glucose. With the help of insulin, a hormone produced in the pancreas, cells throughout the body absorb glucose and use it for energy. If you have diabetes, your body doesn’t use insulin properly. That’s called insulin resistance. When this occurs, blood sugar levels are elevated. Over time, the pancreas can’t make enough insulin to regulate your blood glucose. Too much glucose in the bloodstream can lead to heart disease, kidney disease, nerve damage, and loss of vision.
What are my goals for blood sugar monitoring?
The American Diabetes Association suggests the following blood glucose targets for most nonpregnant adults with diabetes. Work with your medical care team to determine a goal that is right for you.
Blood sugar levels:
- Before meals: 80 – 130 mg/dL (4.4 – 7.2 mmol/L)
- After meals: <180mg/dL (<10 mmol/L)
- A1C level: <7%
Keeping track of diabetes in 2 ways
SHORT TERM – Monitor blood sugar levels To check your blood sugar daily, you may have to rely on a meter or a continuous glucose monitor. Common times to check blood sugar are before a meal (fasting) or two hours after a meal. Talk with your medical care team about how often and when you should check your blood glucose and what your target numbers should be. | LONG TERM – Check hemoglobin A1C Your physician can help you track your diabetes long-term by ordering a hemoglobin A1C test, which indicates your average blood sugar level over the past three months. As a person with diabetes, your A1C goal will likely be <7%. |
Take control of diabetes management
While managing blood sugar is important, maintaining or improving quality of life is essential to wellbeing. By learning about the role of food and nutrition in diabetes management, individuals can help empower themselves to improve their dietary freedom. It can be as simple as making healthy food swaps or building healthy habits. For example, using brown rice instead of white rice, drinking water instead of soda or simply cutting down portion sizes. Many respected diabetes associations, like the American Diabetes Association also endorse the use of diabetes-specific formulas (DSF) as meal replacements to help diabetes management.
- DSF is a nutritious drink that supports diabetes management and provide complete and balanced nutrition for people with diabetes.
- Slowly digestible carbohydrates in DSF help promote satiety and increase secretion of Glucagon-like-peptide-1 (GLP-1)1 which encourages insulin secretion to support better glucose control.2
- Scientific studies have shown that myo-inositol helps to improve insulin sensitivity, leading to better glucose control. 3-5
Reference:
- Devitt AA, et al. Journal of Diabetes Research & Clinical Metabolism 2012;1:20.
- Lim GE, et al. Diabetes 2006;55(Suppl. 2):S70-S77.
- Fraticelli F, et al. Acta Diabetologica. 2018;55:805-812.
- Guo X, et al. J Diabetes Complications. 2018;32(3):342-348.
- Pintaudi B, et al. Int J Endocrinol. 2016;2016:9132052.
Article by:
![]()
MAL.2020.5265.GLU.1
Latest Health Info
Unpacking Lactose Issues: Intolerance, Deficiency, and Malabsorption Explained
Ever wonder why some people, or even yourself, are suffering from lactose intolerance? Lactose, the primary sugar in milk and ...
Detect to Protect: Why Cancer Screening Matters
Cancer is a complex group of diseases characterised by the uncontrolled growth and spread of abnormal cells in the body. ...
Get Vaccinated: Protecting Lives, One Shot at a Time
Vaccines are among the most powerful tools in medicine, saving millions of lives by preventing serious diseases. From children to ...